Piles, Fistula & Fissure
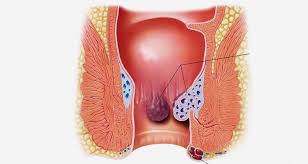
Piles (Hemorrhoids)
Hemorrhoids, commonly known as piles, are swollen and inflamed veins located in the anus and lower rectum that represent one of the most prevalent digestive complaints affecting the adult population worldwide. By the age of fifty, approximately half of all adults will have experienced the characteristic itching, discomfort, and bleeding that signal the presence of hemorrhoids, making this condition an extraordinarily common yet frequently undertreated source of significant personal distress and reduced quality of life. The condition arises when the veins surrounding the anal canal are subjected to increased pressure, causing them to stretch, bulge, and become inflamed in a manner analogous to varicose veins elsewhere in the body. Hemorrhoids are classified into two distinct anatomical types based on their location: internal hemorrhoids, which develop inside the rectum and are generally not visible or palpable from the outside, and external hemorrhoids, which form beneath the skin surrounding the anus and are directly accessible to examination and more likely to cause immediate discomfort and pain.
The symptoms of hemorrhoids vary considerably depending on whether they are internal or external in nature, as well as the severity and duration of the condition. Internal hemorrhoids lying within the rectum typically cannot be seen or felt and usually cause no direct discomfort in their uncomplicated state, but straining or irritation during the passage of stool can damage their delicate mucosal surface and produce painless bright red bleeding noticeable on toilet tissue or in the toilet bowl. In some cases, persistent straining can force an internal hemorrhoid to protrude through the anal opening, a condition known as a prolapsed hemorrhoid, which introduces pain, irritation, and a sensation of incomplete evacuation to the clinical picture. External hemorrhoids, situated beneath the perianal skin, tend to produce more immediately noticeable symptoms including itching, irritation, swelling, and a palpable lump near the anus that may be sensitive or painful to touch. In certain cases, blood may pool within an external hemorrhoid and form a clot known as a thrombosed hemorrhoid, causing a sudden and often severe intensification of pain, swelling, and inflammation that may require prompt medical intervention for relief.
Causes and Risk Factors of Hemorrhoids
The fundamental mechanism underlying hemorrhoid formation is the sustained elevation of pressure within the veins of the lower rectum and anal canal, which causes these vessels to progressively stretch, weaken, and eventually bulge into the surrounding tissue in the characteristic pattern of hemorrhoidal disease. A variety of lifestyle, physiological, and anatomical factors contribute to this pressure elevation, with straining during bowel movements being among the most significant and modifiable contributors to hemorrhoid development. Prolonged sitting on the toilet, chronic constipation or diarrhea, obesity, pregnancy, anal intercourse, and a diet consistently low in fiber all represent well-established risk factors that individually or collectively increase the likelihood of developing symptomatic hemorrhoids. The role of a low-fiber diet is particularly important to appreciate, as insufficient dietary fiber leads to the production of hard, compacted stools that require greater straining effort to pass, directly generating the elevated intravenous pressure that initiates hemorrhoid formation.
Advancing age is another significant and unavoidable risk factor for hemorrhoid development, as the connective tissues and supportive structures that anchor and stabilize the veins of the rectum and anus naturally weaken and lose their elasticity over the course of decades. This age-related tissue deterioration means that the veins become increasingly susceptible to the effects of pressure and are progressively less able to return to their normal position after episodes of straining or increased intra-abdominal pressure. Pregnancy represents a particularly important physiological context for hemorrhoid development, as the growing uterus exerts sustained direct pressure on the rectal veins while simultaneously elevating intra-abdominal pressure throughout the duration of gestation. Fortunately, the majority of hemorrhoid sufferers can achieve meaningful and lasting symptom relief through a combination of conservative home treatments and targeted lifestyle modifications including increased dietary fiber intake, adequate hydration, avoidance of prolonged straining, and the adoption of regular physical activity, with more invasive procedural or surgical interventions reserved for cases that prove refractory to these initial management strategies.
Anal Fissure
An anal fissure is a small but often intensely painful tear in the thin moist tissue lining the anus, known as the mucosa, that most commonly arises as a direct consequence of passing hard, large, or particularly difficult stools during a bowel movement. Despite its small physical size, an anal fissure can produce a disproportionately severe degree of pain due to the exceptionally rich nerve supply of the anal region and the tendency of the tear to trigger intense spasms in the anal sphincter muscle, the ring of muscle that controls the opening and closing of the anus. These sphincter spasms not only amplify the pain experienced during bowel movements but also reduce blood flow to the already injured tissue, creating a self-perpetuating cycle of poor healing, repeated tearing, and ongoing spasm that can significantly delay the natural recovery process. While anal fissures are particularly common in young infants, they can affect individuals across all age groups and both genders, and the condition is far more prevalent in the general population than is widely recognized given the understandable reluctance of many sufferers to seek medical attention for symptoms in this sensitive anatomical region.
The clinical presentation of an anal fissure is typically quite distinctive and recognizable, making diagnosis relatively straightforward in most cases based on the characteristic symptom pattern alone. The hallmark symptom is sharp, severe pain during bowel movements that does not resolve immediately after defecation but instead persists and may continue for up to several hours afterward, a feature that reliably distinguishes anal fissure pain from the milder discomfort associated with hemorrhoids. Bright red blood on the stool or toilet paper following a bowel movement is another consistent finding, accompanied by itching and irritation around the anus that adds a further layer of discomfort to the patient's daily experience. Physical examination typically reveals a visible crack or tear in the perianal skin, and in some chronic cases a small lump or skin tag may develop adjacent to the fissure as a result of repeated cycles of injury and attempted healing. The majority of acute anal fissures resolve spontaneously within four to six weeks with conservative management including stool softeners, increased dietary fiber and fluid intake, topical anesthetic creams, and sitz baths, while chronic fissures that fail to heal with these measures may ultimately require medical treatment with muscle-relaxing agents or minor surgical intervention to achieve lasting relief.
