Gastric Surgery
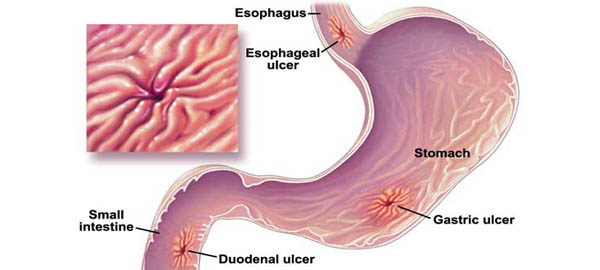
Gastric Ulcer
Food travels down the esophagus into the stomach, where acid is produced to help digest food before it moves into the duodenum and small intestine, where enzymes from the pancreas break down and absorb nutrients. A gastric ulcer, also known as a stomach ulcer or peptic ulcer, occurs when the protective mucous lining of the stomach is damaged by excess acid, leaving the underlying tissue exposed and creating a small, crater-like sore on the inner wall of the gut. This condition falls under the broader category of peptic inflammation, which can also affect the duodenum and lower esophagus depending on where the acid-related damage occurs.
The most common symptom of a gastric ulcer is a burning abdominal pain felt anywhere between the navel and breastbone, which tends to worsen when the stomach is empty, flares at night, and is temporarily relieved by food or acid-reducing medications. In more severe cases, patients may experience vomiting of red or black blood, dark or tarry stools, unexplained weight loss, nausea, and appetite changes. The primary causes include infection with Helicobacter pylori bacteria, which inflames the stomach lining, and the regular use of pain-relieving medications such as aspirin and ibuprofen, which erode the mucous barrier. Additional risk factors include smoking, which amplifies H. pylori damage, and alcohol consumption, which irritates the stomach lining and increases acid production.
Duodenal Ulcer
A duodenal ulcer is a type of peptic ulcer that develops on the inner lining of the duodenum, the upper portion of the small intestine where stomach acid flows in along with partially digested food. Like gastric ulcers, duodenal ulcers form when the balance between acid production and the protective mucous lining is disrupted, allowing acid to eat away at the exposed tissue and create a painful open sore. The condition shares many of its root causes with gastric ulcers, particularly H. pylori infection and frequent use of nonsteroidal anti-inflammatory drugs, making it the most common form of peptic ulcer disease overall.
The symptoms of a duodenal ulcer closely mirror those of a gastric ulcer, with burning pain in the upper abdomen being the hallmark complaint, often occurring when the stomach is empty or during nighttime hours and temporarily relieved by eating or taking antacid medications. Severe complications, though less common, can include significant gastrointestinal bleeding manifesting as blood in vomit or black tarry stools, as well as perforation of the intestinal wall, which constitutes a surgical emergency. Because the symptoms tend to disappear and return cyclically over days or weeks, many patients delay seeking medical attention, unknowingly allowing the ulcer to deepen and increasing the risk of life-threatening complications if left untreated.
Surgery for Cancer of the Stomach
Surgical intervention for stomach-related ulcer complications, while rarely the first line of treatment given the effectiveness of modern medications, becomes necessary in specific circumstances where medical therapy has failed or life-threatening complications have developed. Surgery is indicated for intractable peptic ulcers that do not heal after exhaustive medical treatment and lifestyle modification, as well as for dangerous complications such as severe bleeding, perforation of the stomach wall, or obstruction of the digestive tract that prevents normal food passage. The overarching goal of surgical management is to reduce acid production, restore normal digestive function, and eliminate the conditions that allow ulcers to persist or recur.
The surgical procedures employed in the treatment of ulcers typically involve one or a combination of three techniques tailored to the individual patient's condition and the severity of disease. Vagotomy involves cutting one or more of the nerves supplying the stomach to reduce acid secretion, while pyloroplasty widens the outlet at the bottom of the stomach to improve gastric emptying and reduce acid pooling. In the most severe cases, a partial gastrectomy — the surgical removal of a portion of the stomach — may be performed to eliminate the acid-producing tissue responsible for ongoing ulceration. The treatment of underlying H. pylori infection in conjunction with surgery has dramatically improved long-term outcomes by preventing the majority of ulcers from recurring after the procedure.
Fundoplication
Fundoplication is the gold standard surgical procedure for treating gastroesophageal reflux disease, a chronic condition in which stomach acid repeatedly backwashes into the esophagus due to a malfunctioning lower esophageal sphincter. Under normal circumstances, this sphincter muscle remains contracted between swallows, effectively sealing the esophagus from the stomach and preventing acid reflux. In patients with GERD, however, the sphincter is either weakened or relaxes inappropriately, allowing acid to escape upward and cause inflammation, heartburn, pain, and potentially serious long-term complications such as scarring, stricture formation, and Barrett's esophagus if left untreated.
During the fundoplication procedure, the surgeon takes the uppermost portion of the stomach, known as the fundus, and wraps it around the lower end of the esophagus and the dysfunctional lower esophageal sphincter, securing it in place with sutures in a technique called plication. This wrap effectively reinforces and recreates the natural pressure barrier at the esophagogastric junction, significantly increasing resistance to acid reflux and restoring the protective function that the weakened sphincter can no longer provide on its own. The procedure can be performed using minimally invasive laparoscopic techniques in most patients, offering faster recovery times and reduced postoperative discomfort compared to open surgery, while delivering durable long-term relief from the debilitating symptoms of GERD and halting the progressive esophageal damage caused by chronic acid exposure.
