Pancreatic Surgery
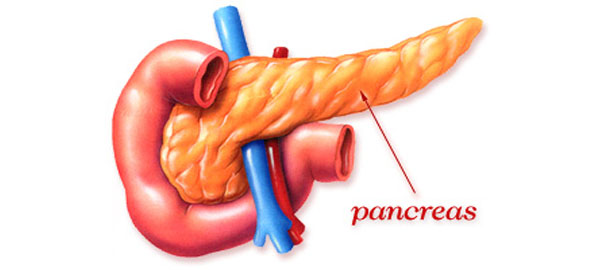
Pancreatic Surgery - Pancreatitis
Pancreatitis is a condition characterized by inflammation of the pancreas, a long flat glandular organ situated behind the stomach in the upper abdomen that serves two critically important physiological functions. The first is an exocrine function, in which the pancreas produces powerful digestive enzymes that are released into the small intestine to break down proteins, fats, and carbohydrates consumed in food. The second is an endocrine function, in which the pancreas produces hormones, most notably insulin and glucagon, that regulate the body's processing and utilization of glucose, making it an indispensable organ for maintaining stable blood sugar levels. When the pancreas becomes inflamed, these normal functions are disrupted, and the digestive enzymes that are ordinarily released into the intestine may become prematurely activated within the pancreas itself, causing the organ to essentially begin digesting its own tissue, a process that underlies much of the pain and damage associated with this condition.
Pancreatitis presents in two clinically distinct forms, each with its own pattern of onset, duration, and severity. Acute pancreatitis appears suddenly and typically lasts for a period of days, presenting with upper abdominal pain that frequently radiates through to the back, worsens after eating, and is accompanied by nausea, vomiting, and tenderness upon touching the abdomen. While mild cases of acute pancreatitis may resolve on their own without specific treatment, severe episodes can escalate rapidly into life-threatening complications including pancreatic necrosis, infection, organ failure, and systemic inflammatory response syndrome. Chronic pancreatitis, by contrast, develops gradually over many years as a result of repeated bouts of inflammation or persistent injury to the pancreatic tissue, manifesting as persistent upper abdominal pain, chronic indigestion, unintentional weight loss, and the passage of oily, foul-smelling stools known as steatorrhea — a direct consequence of the pancreas losing its ability to produce sufficient digestive enzymes to properly absorb dietary fats, leading to their excretion in an undigested form.
Pancreaticoduodenectomy (Whipple Procedure)
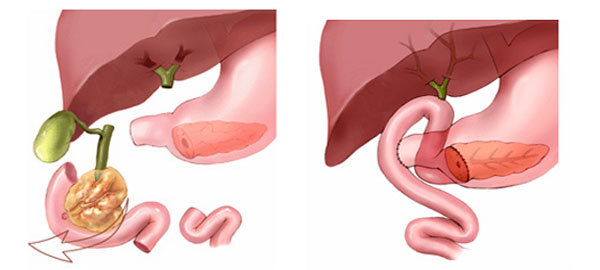
The Whipple procedure, formally known as pancreaticoduodenectomy, is the most commonly performed and most technically demanding surgical operation for the removal of tumors located in the head of the pancreas, and it represents one of the most complex procedures in all of abdominal surgery. During the standard Whipple procedure, the surgeon systematically removes several interconnected anatomical structures, including the head of the pancreas, the gallbladder, a portion of the duodenum representing the uppermost section of the small intestine, a small part of the stomach known as the pylorus, and the lymph nodes in the vicinity of the pancreatic head. A variation of this operation known as the pylorus-preserving Whipple procedure follows the same general principles but deliberately leaves the bottom portion of the stomach intact, which some surgeons believe offers advantages in terms of postoperative digestive function and nutritional recovery. In both versions of the procedure, the operation is extensive and technically intricate, typically lasting between six and ten hours, after which the surgeon meticulously reconnects the remaining portions of the pancreas and digestive organs to restore the normal flow of pancreatic enzymes, bile, and stomach contents into the small intestine to support digestion.
The postoperative course following a Whipple procedure is complex and requires careful monitoring for a range of potential complications that can significantly affect recovery. The most frequently encountered complication is delayed gastric emptying, a condition in which the stomach takes an abnormally prolonged time to empty its contents into the small intestine, typically resolving within seven to ten days as the stomach gradually resumes normal function.
When delayed gastric emptying persists beyond this window, supplemental nutrition delivered through a feeding tube may be initiated to maintain the patient's nutritional status while the stomach recovers, a process that can extend for several additional weeks in some cases. The most serious and potentially life-threatening complication is abdominal infection resulting from leakage at the site where the remaining pancreas has been surgically connected to the intestine, an occurrence seen in approximately ten percent of patients that is generally managed through a combination of drainage tubes, antibiotic therapy, and supplemental tube feedings. Beyond the immediate postoperative period, patients who have undergone the Whipple procedure may experience lasting long-term effects including chronic digestive difficulties stemming from the significant alterations made to the normal anatomy and function of the upper gastrointestinal tract.
Longitudinal Pancreaticojejunostomy (Puestow Procedure)
The Puestow procedure, also referred to as the Puestow-Gillesby procedure or pancreaticojejunostomy, is a specialized surgical technique designed specifically for the treatment of chronic pancreatitis, a condition in which repeated or sustained inflammation of the pancreas leads to progressive scarring, ductal obstruction, and debilitating chronic pain that significantly diminishes the patient's quality of life. The fundamental principle underlying this operation is the creation of a side-to-side anastomosis — a direct surgical connection — between the main pancreatic duct and a loop of the jejunum, the middle portion of the small intestine, thereby establishing a new and unobstructed drainage pathway for pancreatic secretions that bypasses the areas of stricture and obstruction responsible for the buildup of pressure and the generation of pain within the gland. The surgical technique involves making a longitudinal incision along the length of the pancreas and opening the main pancreatic duct from the head of the organ all the way to its tail in a process described as filleting, after which a prepared loop of small intestine is carefully oversewn to the exposed pancreatic duct to create the drainage connection. When performed in appropriately selected patients with documented ductal dilation and obstruction-related pain, the Puestow procedure can deliver meaningful and durable relief from the chronic pain that so severely impacts the daily lives of patients suffering from long-standing pancreatitis.
A particularly important and clinically significant advantage of the Puestow procedure compared to alternative surgical approaches such as the Frey procedure is its organ-preserving nature, which allows the pancreatic tissue itself to remain largely intact throughout the operation. This tissue-preserving quality is of critical importance in patients who already demonstrate evidence of exocrine insufficiency — an impaired ability to produce adequate digestive enzymes — or endocrine insufficiency — a reduced capacity to produce insulin and regulate blood sugar — as a consequence of their chronic pancreatitis. Removing additional pancreatic tissue in such patients, as some alternative procedures require, could potentially worsen these insufficiencies and lead to more severe nutritional malabsorption or the development of diabetes, making the Puestow procedure a particularly thoughtful and well-suited surgical choice for this vulnerable subset of patients. The overall goal of the procedure is not to cure chronic pancreatitis, which remains an irreversible condition, but rather to significantly improve the patient's pain levels, preserve as much pancreatic function as possible, and restore a meaningful quality of life that chronic, unrelenting pancreatic pain would otherwise make impossible to achieve.

